- Surgical
- Cosmetic Treatments
- One Longevity
- Shop
- About
- Gallery
- Contact
- Book now
Breast Augmentation
Breast augmentation stands out as one of the most sought-after cosmetic procedures in Australia. This entails the placement of a breast implant in each breast, enhancing their shape, volume, and overall proportion to the body. At One Cosmetic, we recognise the importance of this choice, and we’re here to offer our insight to assist you in making the best decision for your body. Additionally, we provide guidance throughout your breast augmentation recovery and aftercare journey.
Our commitment to you, lies in having open and honest communication, ensuring a clear understanding of the procedure, potential risks, and expected outcomes. Our skilled specialist plastic surgeons will walk you through various implant options and incision placements, offering personalised recommendations for you!
| Results | Last 10-15 Years |
|---|---|
| Surgery Time | 1 hour |
| Off-Work | 7 - 14 days |
| Exercise | Limited for 6 weeks |
A breast augmentation (mammoplasty) is a surgical procedure that uses implants to change the size and shape of the breasts.
This procedure can be used to:
- Increase the overall size of the breasts.
- Alter breast shape or volume, for instance, following pregnancy or significant weight changes.
- Address breast asymmetry (a difference in size or shape between the breasts).
It is crucial for patients to have a clear understanding of both the potential outcomes and the significant risks involved with this surgery before making a decision. A personal consultation is necessary to discuss your specific situation and determine your suitability for the procedure.
The Implant
At One Cosmetic, we use the highest quality breast implants available on the Australian market — Motiva and Mentor breast implants. Both brands come in a range of shapes, sizes and profiles. Each silicone implant is filled with a cohesive gel that holds together uniformly and retains a natural give that better resembles breast tissue. During your consultation, your surgeon will be able to determine what implant is most suitable for you.
Motiva breast implants are smooth breast implants that our plastic surgeons commonly use during breast augmentation surgery. We chose Motiva breast implants due to their ongoing studies and safety measurements. Motiva breast implants come in a round and ergonomic shape.
Round – the round implant is uniformly round in shape and holds the firmness even during movement. Patients commonly opt for this implant to achieve the maximum upper pole fullness.
Ergonomic – The ergonomic implant is characterised by its ability to be dynamic with the body. Meaning that as you move, so will the implant. While lying down the implant will hold a more rounded shape, however when standing the implants will appear to be more teardrop.
Mentor are one of the longest implant providers in Australia and each year thousands of women receive breast surgery using Mentor implants. Like Motiva, Mentor breast implants also come in two shapes. First being a round implant and second being a teardrop implant.
Round –Round implants are characterised by their circular and symmetrical shape, often yielding more pronounced results in breast augmentation.
Teardrop – Teardrop Breast Implants, also referred to as Anatomical Implants, aptly mirror the shape of a teardrop. These implants exhibit a tapered and less full upper portion, while the lower part is rounder, fuller, and wider.

Before deciding whether to pursue breast augmentation surgery, you may be a good candidate for surgery if:
- You want to alter the appearance of your breasts
- You have a minimal amount of breast tissue and wish to have more
- You are well-supported and have realistic expectations of the surgery
- You’re able to take sufficient recovery time off of work
- You are a non–smoker or are willing to abstain from smoking at least 8 weeks before surgery and 8 weeks post-surgery
- You are 18 years or older
- You understand there are risks involved and we cannot guarantee outcomes.
Double Bay Day Hospital
Macquarie University Hospital

The Surgery Process
The decision to undertake any type of elective surgery should be a well thought and long process. We do not recommend rushing into any procedures. Below is a guide on the surgery process and the risks involved.
The first step in finding out more about breast augmentation surgery is to schedule a private consultation. In this consultation, you will meet directly with your specialist Plastic Surgeon. This gives you an opportunity to discuss your concerns and get all of your questions answered. Before you go into your consultation, you will have our Vectra 3D imaging completed with our breast nurse. The Vectra system allows you to visualise what your post surgery results will look like.
To book a surgery date you can contact our team after a face to face consultation has been completed. You must wait 7 days from the consultation to book a procedure.
During the consultation, your surgeon will delve into your medical background, inquiring about your medical history and any history of substance abuse, tobacco, or alcohol use. It’s essential to bring along a comprehensive list of all medications and supplements you are currently taking. The consultation includes a thorough examination of your complete and accurate medical history, where you’ll disclose any past surgeries, procedures, or complications you’ve encountered.
These detailed information equips your Surgeon to make an informed decision about your general health and assess whether you are an ideal candidate for the procedure. Fortunately, the majority of individuals meet the criteria for the intended procedure.
At the end of your consultation, your surgeon will provide personalised recommendations regarding the best course of action to help you achieve your desired outcome from breast augmentation surgery. Every patient is unique, and results will vary from person to person.
While inspiration images can be helpful in understanding your goals, it’s important to understand that we cannot guarantee your results will exactly match those images. This is a crucial consideration before proceeding with breast augmentation surgery.
Choosing the right breast implant size is one of the most challenging decisions in the augmentation process. During your consultation, your surgeon will take detailed measurements and assess factors such as your existing breast tissue and overall breast shape to determine which implant types may be most suitable for you.
Although we will provide guidance based on your anatomy and goals, the final decision regarding implant size ultimately rests with you.
Once you’ve booked your surgery date, a pre surgery appointment will be scheduled 4 weeks prior to your date. This is your chance to meet with your surgeon again, ask any further questions, go over the surgery plan and take some images. This appointment ensures you’re well prepared for the upcoming surgery date.
The night before and the morning of your breast surgery, you’ll need to adhere to certain guidelines. Typically, you should refrain from eating and drinking fluids after midnight, as is common with many surgical procedures.
Depending on your surgeons advice, you may be allowed to take specific medications with a small sip of water, such as beta-blockers or cholesterol medications. To minimise the risk of infection, it is recommended to shower with an antimicrobial soap both the evening before and on the morning of your surgery. Be gentle, during the cleansing process to avoid irritation.
For hygiene reasons, it’s advised not to wear nasal, nipple or facial piercings to the hospital to prevent loss and potential bacterial contamination.
Upon arrival at the hospital, nursing staff will conduct necessary checks, and you’ll have an opportunity to meet with your surgeon just before the procedure to ensure you feel prepared. In the operating room, you’ll be administered the appropriate anaesthesia.
To minimise visible scars, incisions are typically made in the fold of the breast. Your surgeon will carefully prepare the breast pocket for the implant. Once ready the breast implant will be placed inside the breast space. Breast augmentation surgery usually take 1-2 hours. Once completed the breast pocket will be closed and a dressing will be applied to the area, you will be moved to the recovery room.
All sutures are dissolvable, therefore you will not need to have sutures removed post surgery.
Many patients find reassurance in knowing that breast augmentation is typically performed as an outpatient procedure under general anaesthesia. This means most patients are able to regain mobility within a few hours after surgery.
It’s normal to experience some soreness during the first two weeks following the procedure, and during this time, strenuous physical activity should be avoided to support proper healing.
You will be provided with a La Twin post-surgical recovery bra, which should be worn for 6 to 12 weeks as part of your healing process. Wearing the appropriate post-surgical garment is an essential component of recovery. The La Twin compression bra is specifically designed to reduce swelling, minimise the risk of implant displacement, and support scar management.
Postoperative prescriptions, such as antibiotics to help prevent infection and pain medication for comfort, are often provided in advance. Following all post-operative care instructions closely is crucial for achieving the best possible outcome.
Surgical risks such as bleeding or infection
Fluid accumulation around the implant after surgery
Allergic reaction to suture materials, tape adhesive or other medical materials and lotions
Changes in breast and nipple sensation
Temporary or permanent areas of numbness
Wrinkling of the skin over the implant
Keloid, or lumpy scar tissue, which is pink, raised and irregularly shaped. These scars may be inflamed and itchy. There are several possible sites for the incision. Discuss this with your surgeon
Inappropriate implant size
Asymmetry (unevenness) of the breasts
Calcium deposits in the scar capsule around the implant
Granulomas, or lumps in local lymph node tissue formed by leaking silicone
Breastfeeding difficulties, including reduced milk supply
Reduced effectiveness of breast cancer screening, since an implant may hide breast tissue (and tumours) during a mammogram
Movement of the implants from their original position
Further surgery to treat complications
Risks of anaesthesia including allergic reaction or potentially fatal cardiovascular complications such as heart attack
A blood clot in the deep veins of the legs (deep vein thrombosis), which can move to the lungs (pulmonary embolus) or to the brain and may be life threatening
- unsatisfied with surgery outcome
- Breast implant illness
- Breast Implant Associated-Anaplastic Large Cell Lymphoma (BIA-ALCL)
- Reduced effectiveness of breast cancer screening, as an implant may hide breast tissue (and tumours) during a mammogram
- Movement of the implants from their original position
- Further surgery to treat complications
After surgery our recovery specialists will given post-op instructions. It is important to follow carefully. You will be provided with a script for medication, which you will need to purchase after surgery and instructions on when to take the medication over the days ahead. You will be discharged from hospital when your companion picks you up from the hospital. All patients must have a companion to stay with them for 72hours following surgery.
The first week after surgery you should stick to gentle day-to-day activities. This includes minimal house duties, no lifting, staying home as much as possible and sleeping in an elevated position. Commence postoperative exercise (instructions given post surgery).
In the second week of recovery try not to raise your blood pressure too much and still sleep in an upright position. Patients will also be required to attend a postoperative appointment at our office in week 2. this will be scheduled prior to surgery.
In week 2 patients may:
Commence a light walk
Return to work in week 2 if you have an office job with little physical activity
Avoid sexual intercourse
Start driving provided they are not taking any pain medication. We also recommend waiting 3 days for the medication to be out of your system.
Weeks 3 – 5 patients with more physical jobs can return to work.
In weeks 3-5 patients may:
Start getting into a light exercise routine, using lower body
Start doing more physical household duties
In weeks 6-8 patients may:
Commence normal exercise routine and duties. Please note, do not push yourself into being back into your pre surgery routines.
Swimming, bathing running, yoga, stretching, spin class and Pilates
Stop wearing compression bra (Textured Mentor implants)
At this stage patients are mostly fully recovered and sutures are absorbed. Patients should always wear a supportive bra when exercising or performing physical activity. For all patients with teardrop breast implants we recommend that you do not ever go back to using or exercising chest muscles heavily as teardrop implants can rotate.
In weeks 9-12 patients may:
Contact sport
Boxing and upper body exercise
Stop wearing compression bra (smooth Motiva implants)
Monitoring your safety for life
With any surgery, follow-up care is essential. So, we provide patients with ongoing support through our lifelong follow-up. All patients who have breast augmentation in Sydney with us will receive regular post-operative check-ups to avoid any potential complications in the medium to long term. It is essential to understand that a medical device has been used and must be monitored when the patient has the implant.
The Breast Implant Registry (BIR) is a public health initiative focusing on patient safety. The Registry collects relevant patient, surgeon, procedural and implant data relating to breast implants. We register all patients post surgery. The Registry is administered by the Australian Society of Plastic Surgeons (ASPS).
Motiva
All Motiva implants are covered against rupture by the Always Confident Warranty, for the lifetime of the device, and by Product Replacement Policy against capsular contracture, Baker grades III and IV for a period of 10 years.
Furthermore, Motiva offer Extended Warranty Programs, which you may decide to participate according to your personal case:
- For Motiva Implants®without Q Inside Safety Technology™ our 2Y Motiva Program™
- For Motiva Implants®with Q Inside Safety Technology™ our 5Y Motiva Program™
In addition to the replacement product, these programs will support you with financial assistance for each affected implant, applicable to the cost of the revision surgery in the event of a warranty claim for rupture or capsular contracture Baker grades III and IV.
Mentor
All recipients of MENTOR® Breast Implants are automatically enrolled in the MENTOR® Promise Protection Plan. Should a confirmed rupture or deflation occur, the patient will receive up to two replacement breast implants of the same style or like style at no additional charge for the lifetime of the patient.
If a rupture occurs within 10 years of surgery, the patient may also be eligible for financial assistance for surgical costs not covered by insurance. Additional complications are also covered for 10 years with free product replacement.
Implantation of the MENTOR® Breast Implants, as well as any subsequent procedures, must be in accordance with current Mentor Product literature and accepted plastic surgical procedures by appropriately qualified licensed physicians for product to qualify for replacement under the Mentor Product Replacement Policy.
Frequently Asked Questions
We regularly get asked about our procedures, so we have put together a couple of questions we get asked on a regular basis. If there is something else you would like to know, please get in touch!
Individual cases may vary but generally, mothers can breastfeed after having breast augmentation. However, some women do experience reduced nipple sensation following breast augmentation surgery making it difficult to trigger the milk let down reflex. Some women may also experience reduced milk supply.
Unfortunately, breast implants will not last forever. Life expectancy is estimated at 10-15 years.
As this is a cosmetic procedure, there is no Medicare rebate or health insurance cover available.
yes, scars are apart of this procedure. The scar is about 3-4cm under each breast fold. With care and diligence the scar will fade over time, however there will always be some trace of a surgical scar on the body.
The Mentor implants come in round or teardrop shapes — the round shapes are well-suited to patients who are happy with their breast shape and want to increase their breast size. In contrast, the teardrop shape provides a more natural look that may be ideal for patients with slightly droopy breasts, such as post-pregnancy, breastfeeding or with weight loss. Round Motiva breast implants give a fuller, round appearance. When standing, the lower pole of the breast will be fuller as this implant has more movement.
Our team will assess your breast composition, listen to your goals and advise on the best implant size and shape for your body during your initial consultation.
After the breast augmentation procedure, our patients are taken to recovery for 2–4 hours with our recovery care specialists and can travel home that same evening. Our post-op specialists will provide you with post-op instructions to ensure a smooth recovery.
To book your personal consultation, please contact our team on 1800 678 679 or info@onecosmetic.com.
Our consultation dates are normally booked 1-2 months in advance.
Smoking before or after surgery is strictly forbidden as it will significantly impair healing and increase the risk of complications. Here’s why:
Reduced Oxygen Supply: Smoking constricts blood vessels and decreases the amount of oxygen that reaches tissues. Oxygen is essential for wound healing, so smoking can delay recovery, increasing the risk of infections and poor scar formation.
Increased Risk of Complications: Smoking elevates the likelihood of surgical complications, such as poor wound healing, tissue death (necrosis), blood clots, and respiratory issues during and after surgery. Smokers may also have a higher risk of infections and complications with anaesthesia.
Impaired Immune System: Smoking weakens the immune system, making it harder for your body to fight off infections, which are already a risk after surgery.
Prolonged Recovery: The toxins in cigarettes can extend recovery time, making you more vulnerable to post-operative issues like pain, swelling, and prolonged bruising.
To promote the best healing and minimise risks, it is essential to stop smoking 8 weeks before and after surgery.
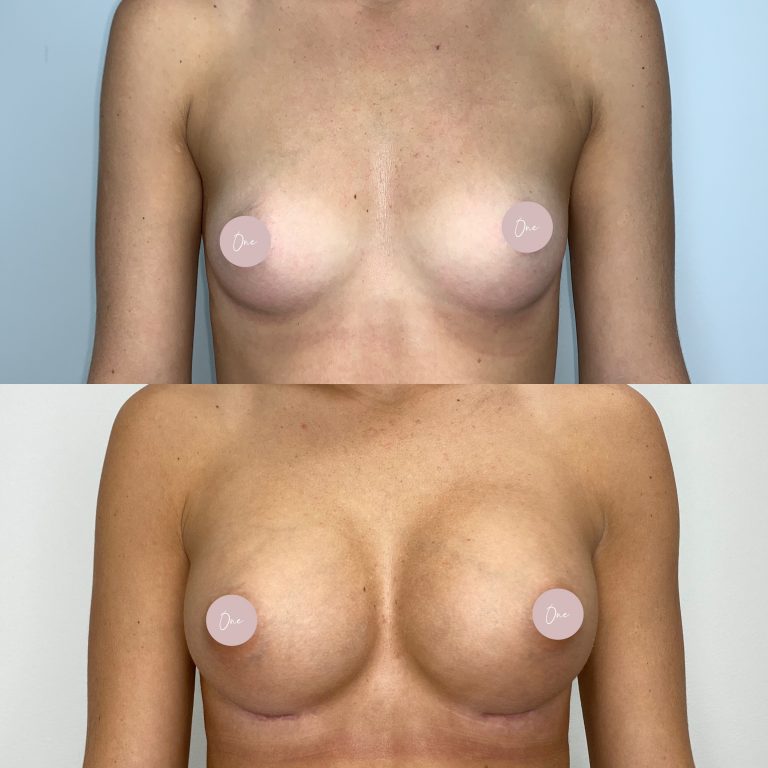
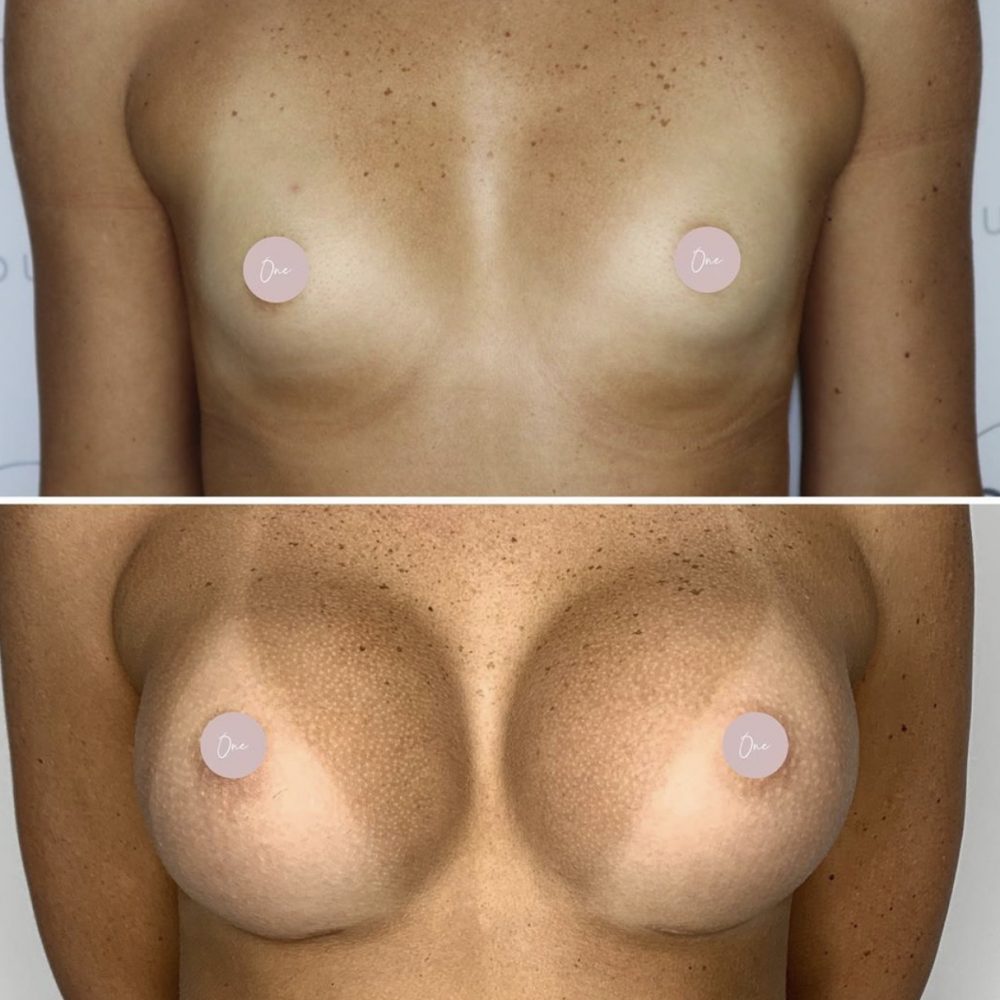
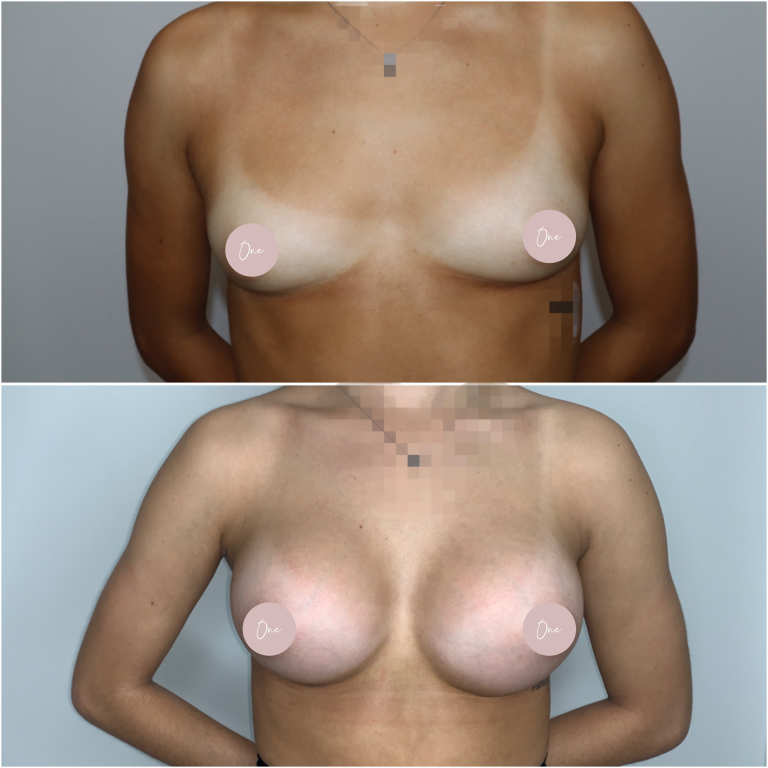
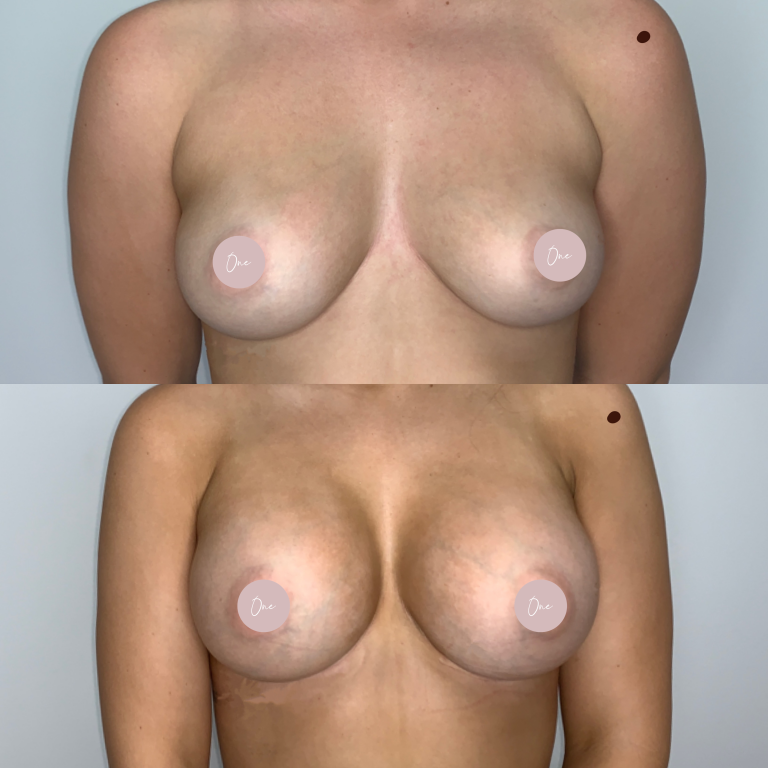
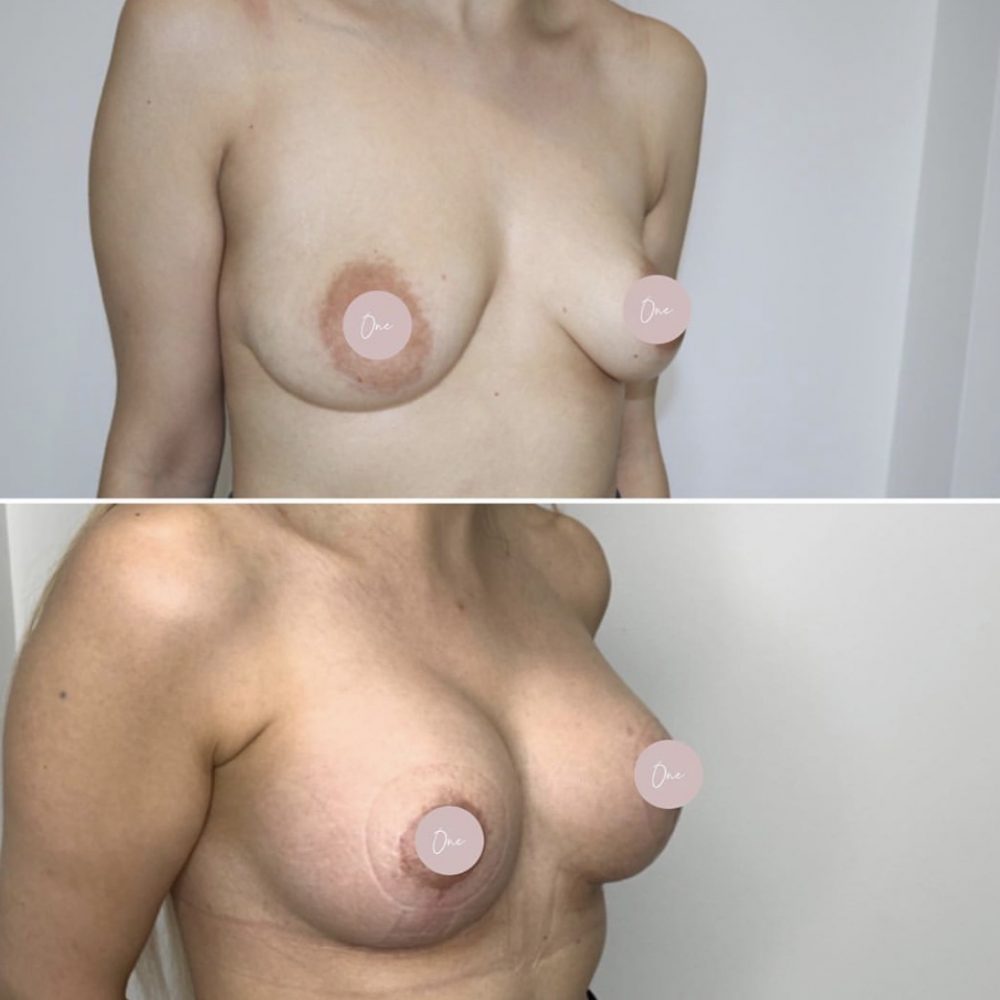
Before & After
The images below contain content of an adult nature.
If you are under 18 years of age, please leave the site now.
Are you over 18?
Our site requires you to be 18 years or older to enter
Lucy McDermid
PATIENT Coordinator
Christie Cameron
Award Winning Dermal Therapist
Having worked across some of the world’s most luxurious spas and leading clinical skin practices, Christie is known for her uncompromising standards, innovation, and results driven approach. Her treatments seamlessly integrate advanced skin science, product chemistry, and biohacking inspired techniques with wellness led practices that support the parasympathetic nervous system through breathwork and mindfulness. Blending ancient techniques with modern day technology, the result is a deeply restorative yet clinically effective experience designed to optimise skin health while delivering visible transformation.
Christie’s elevated approach to treatment and exceptional client experience has attracted a long list of clientele, including celebrities, influencers, beauty editors, media personalities, and high profile individuals.
Beyond the treatment room, Christie is a published contributor to leading beauty publications and a respected educator, dedicated to shaping the next generation of skin therapists. Through her teaching, she inspires practitioners to unite artistry, innovation, and scientific precision setting a new standard for modern skin health.
Jade Pike
Patient Coordinator
Jade is the friendly and approachable face you’ll first meet at One Cosmetic, dedicated to making each client’s experience smooth and enjoyable. From the moment you book your appointment to the time you leave feeling rejuvenated. With a love for natural beauty, she brings genuine care and intention to every interaction.
Dr. Negin Sedaghat
SPECIALIST BREAST AND GENERAL SURGEON
FRACS MBBS BAS (Phys)(Hons)
Sydney Professional Certificate in Oncoplastic Breast Surgery (USYD)
Full Member BreastSurgANZ
VMO Surgeon BreastScreen NSW
Dr Sedaghat is an Australian-trained Specialist General Surgeon with subspecialisation in Breast Surgery and Breast Surgical Oncology. She is BreastSurgANZ certified in breast surgery and awarded professional certification with distinction in oncoplastic breast surgery from the University of Sydney.
Dr Sedaghat combines her highly qualified and experienced surgical expertise with a compassionate and holistic approach to patient care. In addition to breast implant care, Dr Sedaghat accepts consultations for women seeking comprehensive breast assessment and treatment for a wide range of breast concerns at the welcoming and luxurious environment of One Cosmetic in Double Bay – a valid GP referral at the time of consultation will be needed.
Maree Riitano
Nurse
Maree offers all aesthetic medicine treatments and takes a personalised, multi-modality approach when creating treatment plans. She has a focus on restoring and enhancing her clients’ natural anatomy rather than altering them. Her philosophy is centered on subtle, confident beauty and helping clients feel empowered in their own skin.
Maree stays at the forefront of the industry by regularly attending advanced training and cosmetic conferences, ensuring she brings the latest techniques and highest standard of care to every client.
Ailiya Greaves
Senior Dermal
Throughout her career, Ailiya has built a strong reputation for delivering advanced, results-driven treatments with a focus on safety, precision, and patient care. Her extensive clinical experience spans a wide range of skin concerns, including rosacea, acne, pigmentation, scarring, and age-related changes. She takes pride in creating personalised treatment plans that integrate evidence-based dermal therapies to achieve optimal skin health and natural outcomes.
Currently undertaking a Bachelor of Nursing, Ailiya continues to advance her clinical knowledge and professional capabilities. This additional qualification enhances her holistic approach to treatment, combining nursing principles with her dermal expertise to ensure the highest standards of care.
As a valued member of OC’s Dermal Team, Ailiya is recognised for her professionalism, approachable manner, and commitment to empowering clients to feel confident in their skin. Her dedication to continuous learning, coupled with years of hands-on experience, ensures her clients receive exceptional care and outstanding results.
Katie O'Connor
Practice Coordinator
Katie is passionate about skin and skin health, which is so important when patents are seeking advice on where to start. Katie has also recently been through the surgery process herself, so she can give first hand experience when it comes to any surgery related questions.
Chelsea Scutts
REGISTERED NURSE
Chelsea treatments include anti wrinkle, dermal filler, PDO threads, lip enhancements, Morpheus8 face and body sculpting and much more! She has an eye for natural beauty and enhancing her patients features. She regularly attends seminars to learn new techniques for best practice.
Dr. Louis Wessels
SPECIALIST PLASTIC SURGEON
MBChB | FRACS (Plast) | FCS Plastics (SA) | MAdv Plastic Surgery (Macquarie University) | MMed Plastics (SA)
Dr. Louis Wessels is a highly qualified specialist plastic, cosmetic, and reconstructive surgeon with a particular focus on breast and body surgery, including liposuction.
His practice encompasses the full spectrum of cosmetic and reconstructive procedures, with special expertise in breast surgery. These include primary and revision breast augmentation, breast reduction, breast lift, and tuberous breast reconstruction, as well as body contouring procedures such as abdominoplasty (tummy tuck) and liposuction.
Dr. Wessels completed his medical degree (MBChB) in South Africa, followed by internship and general surgery training in one of the most demanding clinical environments. He subsequently completed both his Fellowship and Master of Medicine in Plastic and Reconstructive Surgery in South Africa, gaining extensive experience across complex reconstructive and cosmetic procedures.
He later completed a second Fellowship in Plastic and Reconstructive Surgery in Sydney, Australia, and was awarded Fellowship of the Royal Australasian College of Surgeons (FRACS) in 2015. Dr. Wessels has published internationally recognised research on breast implant infection and outcomes following breast augmentation surgery.
He subsequently graduated from Macquarie University in the inaugural intake of the Master of Advanced Surgery (Plastic and Reconstructive Surgery), for which he was awarded a scholarship from Johnson & Johnson.
Committed to excellence and innovation, Dr. Wessels regularly attends international conferences and professional development seminars to remain at the forefront of evidence-based practice and advanced surgical techniques. He is the founder and lead surgeon at One Cosmetic.
Professional Memberships and Associations
- Australasian Society of Aesthetic Plastic Surgeons (ASAPS)
- Australian Society of Plastic Surgeons (ASPS)
- Royal Australasian College of Surgeons (RACS)
- International Society of Aesthetic Plastic Surgeons (ISAPS)